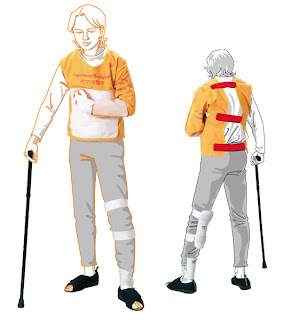
I am father of Ankit from Varanasi. My son is suffering with cerebral palsy since birth. Previously he was not able to walk properly. We had gone through so many treatments from various places and also consulted so many doctors and therapists. Somehow, he started walking with the help of walker. But I was not satisfied with his walking pattern because he was walking with bending his both knees and his both hand also had some problem.

He was having great urge to go school but we were not able to send school due to his physical problem. One day someone ask me to consult Dr. J.K. Jain an orthopedic surgeon in Allahabad. I had consulted him and he suggested me that Ankit needs SEMLS by OSSCS concept, which will help him to relieve his disability and will able to walk nicely. My son had gone through this surgery on 23rd January 2012. After few days physiotherapy has also started.
We stay at Allahabad for 6 month for therapy after surgery. After 3 months of surgery, my son has shown excellent response in walking pattern his hand function also became better. He started walking with two sticks. During this treatment period, we got a nice accommodation at CP Home in Allahabad. Each and every person here is very much familiar. I am very much grateful to Dr. Jain and his team. I am highly satisfied with the whole team of Samvedna.
I am from Raipur, Chattisgarh. I am farmer by profession. My daughter Jyotsna had problem in walking, sitting, standing etc. She was not able to do her own work. I had shown her to so many doctors at different places but there were no positive outcome. I was hopeless. She was making every effort for walking but due to deformity in all four limbs, she was not able to walk.
Then one day I read about camp of Samvedna at Raipur in a newspaper and met Dr. J. K. Jain at a camp in Raipur. Then he said that through an OSSCS surgery and physiotherapy, my daughter’s disability will be restored. I was having lots of financial problem. Dr J K Jain has given assurance for financial support for our daughter surgery. Jain Samvedna trust from Raipur as well as Samvedna , Allahabad is given us assurance for support. Then with lot of hope I took my daughter to Allahabad. Dr. J.K. Jain performed surgery on her. She was undergone surgery in all four limbs by SEMLS. After few days’ of surgery, physiotherapy was started. She started showing positive response within month of surgery.
She was able to put proper pressure upon her entire feet. Now she is able to walk with the help of the sticks. Her hand function became much better. I hope that she will be able to walk without any support and for that we also have to support her a lot.
We got a very good accommodation at Cerebral Palsy Home in Allahabad. I cannot explain response and support given by whole team of Dr J K Jain without much expenditure. Here everybody is very helpful by nature. I am very much grateful to Dr. Jain. The physiotherapy team has also done a really hard work. I am highly satisfied with the whole team of Samvedna and thankful to all of them who have taught my daughter to stand her on her own feet.